|
 DvC2-01 DvC2-01
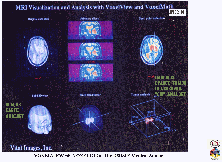
Figure DvC2-01 is from a Vital Images, Incorporated, VoxelGeo software advertisement (presently being developed and marketed by Paradigm Geophysical). It advertises their medical software (VoxelView), from which VoxelGeo was derived. Using MRI technology in this 1990 advertisement, a 3-D opaque human head is examined, virtually, showing the ability to control the opacity (transparency) of the individual Volume-PIXELs (aka, VOXELs) that make up a digital computerized volume. Here, planting a seed in a suspected tumor and performing sub-volume detection is demonstrated. This technique permits an interpreted 3-D opaque tumor to be viewed at any angle (and in animated motion), within a background of transparent VOXELs. This revolutionary 3D medical technology provided the impetus for transforming an unconventionally high-resolution, 2D seismic processing sequence into the patented D3DSP.
Like oil industry workers who deal with hidden targets in the visibly opaque earth, physicians and medical researchers cannot see inside the human body without visualization assistance. Their most common tools of choice are X-ray (Computerized Axial Tomography, or CAT) scans, induced-atomic-nuclei Magnetic-Resonance Imaging (MRI, using an injected paramagnetic dye), and diagnostic ultrasound measurements (medical "D3D seismic"), using both instantaneous snapshots and TV-monitored real-time movies. Positron Emission Tomography (PET scan), using an injected low-intensity-radioactive dye, is becoming another common tool for the medical arts. When a doctor wishes to investigate an object inside an opaque human body, they do not hire RN's to pick peaks and troughs on EKG's. Nor do they contract with processors to calculate MRI attribute volumes, or offer overrides to radiologists to make structure and amplitude maps from CAT scans. This display shows an example of a common use of appropriate medical imaging technology: an MRI intensity data volume of a patient's head. Not only can one "visualize" a 3D sub-volume (geological object), but today's VoxelGeo permits numerous measurement and analysis functions to aid in a quantitative description and evaluation of the a seeded object.
In this published commercial example, the shape of the opaque skulls (lower left) is examined by means of traditional planar slices to identify a suspected high-MRI-radiation-intensity anomaly (or tumor, upper-left and middle). The medical operator then chooses a "seed point", or starting VOXEL, on a slice through a potentially pathological subvolume (upper right). One by one, increasing intensity cutoff values are used and logical "detections" are performed, each time building a common-intensity-object, or CIO, of all VOXELs that are contiguous to the starting VOXEL and that satisfy the criterion that their intensity values are (in this MRI-intensity case) greater than the cutoff value. When the detection cutoff, or threshold, is too low (too relaxed), the detected object will include surrounding normal tissue. To arrive at a "final" 3-D object, the step-by-step, detect-and-evaluate procedure below might be followed (remember that these medical targets are usually high-intensity, whereas the D3DSP more often seeks to "grow" CIOs with relatively low D3D-impedance):
1. Select a "starting VOXEL" within a suspected (prospective?) anomalous sub-volume from any appropriate (horizontal or vertical) slice of data. The goal is to "grow" the sub-volume to some maximum size that represents the size, shape and intensity of the suspected target: in this case, the three-dimensional, potato-shaped tumor, in the lower-right corner of this Figure. The desire is to have the detected, organic-sub-volume contain all of the pathological, "high-intensity" tumor cells, and none of the lower-intensity, normal cells in which it is encased. The D3DSP has an analogous goal, but the geological-sub-volume targets are collections of anomalous "relative acoustic impedance" VOXELs (tiny T'ubes of rock and fluid, some of which may be commercial petroleum reservoirs).
2. Start the first "detection" operation using a detection criterion ("cutoff value") equal to the intensity value of the starting VOXEL. This usually results in the near instantaneous growth (i.e., attaching all contiguous VOXELs whose intensity amplitudes have one thing in "common": they are all greater than or equal [GE] to the cutoff value) of a small, compact, high-intensity sub-volume that is a minimum-volume Common-Intensity Object (a medical CIO). Prior to this first detection run, each intensity amplitude value of every VOXEL in the data volume was "reset" to an even integer (odd values are reduced in amplitude by 1 unit, and even values are not changed). When any one of the starting VOXEL's 26 adjacent VOXELs is found to satisfy the GE criterion, that VOXEL is said to be critically "detected", and the binary number one (1) is added to the VOXEL's formerly even amplitude ... to make it an odd integer, which signifies that it now belongs to the detected CIO.
3. Decrease the cutoff value by one even-valued "step" (two integer values).
4. Interrogate and detect any even-valued VOXEL that is physically outside but adjacent to the now odd-valued CIO. If its amplitude is GE to the new, lower-value cutoff criterion, its amplitude is bumped up to an odd integer (electronically flagged) so that it is now included in the growing surface layer of the all-odd-intensity-values, expanding Common-Intensity Object.
5. Adjust the color and opacity scales of all detected (odd) VOXELs, so that they now form a relatively opaque "common-intensity" object.
6. Evaluate the size, shape, location, and other quantitative attributes of the object.
7. Repeat steps 3-6 until the medical-CIO is too large to represent just the suspected pathological target (e.g., tumor, bone chip, bullet, etc.), whose typical shape is recognizable.
8. Reduce the cutoff value by one step, backing it off from its "overgrown size".
This final medical-CIO is usually the final diagnosed pathological tissue or imbedded material, as judged by an experienced physician or radiologist. It is the "intensity-cutoff interpretation" that will determine the significance (and accuracy) of all the following analyses and measurements, to be used for prescribing treatment or non-treatment. In the lower center and right corner of this Figure, the opaque object is the maximum size, anomalous, three-dimensional sub-volume that could be grown, and is therefore judged to be a "seed-filled" brain tumor, to be virtually measured and evaluated.
In the article seen under the VTV Home Page "Objects vs. Layers" button, the D3DSP "Objects vs. Layers" analogy is compared to both the Wave-Particle Duality and to high-tech medical methods. In comparing these concepts, there is always the risk of seeming to overstate the importance of the D3DSP or seeming to trivialize the W-P Duality or the resulting medical tools. It is clear that the life-or-death importance of this final, volumetric, "intensity-cutoff interpretation" cannot be overstated for the patient. It seems of paramount importance to recognize this one, widely ignored (in the oil and gas industry) fact:
That digital data processing of complex 3D data volumes, always acts as a "pre-interpretation" of the medical- or geological-CIO's imbedded in a data volume.
And this is much more critical in the seismic than in the medical theaters, because there are many more decisions made by a seismic processor (seeking the highest "layered-signal"-to-noise ratio), than by a medical data volume processor, who know from autopsies and text books what their targets look like. The D3DSP contends that this advantage of medical industry processors over petroleum industry processors, is due to a simple the fact that medical workers know their targets are 3D objects, and do not need to work so hard to create a "layered look".
|

